Early Detection
Early Detection
In Cairo Cure, we provide early detection to our patients. Below is an explanation of several types of cancer, and our recommended early detection mechanisms for those types of cancer: Breast Cancer, Cervical Cancer, Lung Cancer, and Colo-rectal Cancer.
Early Detection of Breast cancer
Breast cancer is the most common type of cancer among women in the Middle East. Early detection is the key in the treatment of breast cancer. There are steps you can take to detect breast cancer early when it is most treatable.
Healthy Habits Leading a healthy lifestyle can help you reduce your risk factors for breast cancer and other illnesses. However, all women should perform a self breast-exam each month and any changes or abnormalities should be discussed with a doctor or physician.
- Women age 40 – 45 or older who are at average risk of breast cancer should have a mammogram once a year.
- Women at high risk should have yearly mammograms along with an MRI starting at age 30.
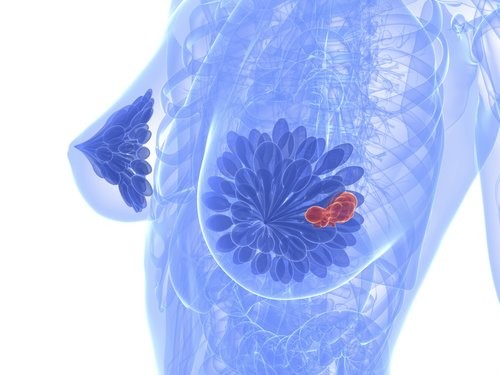
If you suspect any abnormalities, do not hesitate to receive a Clinical Breast Exam or a Mammogram.
The Clinical Breast Exam is performed by a qualified nurse or doctor. The mammogram is the most important screening test for breast cancer. A mammogram is an X-ray of the breast. It can detect breast cancer up to two years before a tumour can be felt by you or your doctor.
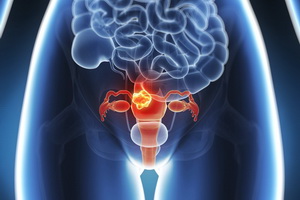
Early Detection of Cervical Cancer
Cervical cancer is that affecting the cervix, which is the lower narrow part of the uterus(womb), that connects it to the vagina(birth canal).Human papillomavirus (HPV) is a virus that is responsible for many cases of cervical cancer.
The best way to find cervical cancer early is to have regular screening with a Pap test (which may be combined with a test for human papilloma virus or HPV). As Pap testing became routine in this country, finding pre-invasive lesions (pre-cancers) of the cervix became far more common than finding invasive cancer. Early detection greatly improves the chances of successful treatment and can prevent any early cervical cell changes from becoming cancerous.
- All women should begin cervical cancer screening at age 21.
- Women aged 21 to 29, should have a Pap test every 3 years.
- Beginning at age 30, the preferred way to screen is with a Pap test combined with an HPV test every 5 years. This is called co-testing and should continue until age 65.
- Another reasonable option for women 30 to 65 is to get tested every 3 years with just the Pap test.
- Women who are at high risk of cervical cancer because of a suppressed immune system (for example from HIV infection, organ transplant, or long-term steroid use) or because they were exposed to DES in utero may need to be screened more often. They should follow the recommendations of their healthcare team.
When to stop screening?
Women over 65 years of age who have had regular screening in the previous 10 years should stop cervical cancer screening as long as they haven’t had any serious pre-cancers found in the last 20 years.
Also, women who have had a total hysterectomy (removal of the uterus and cervix) should stop screening.
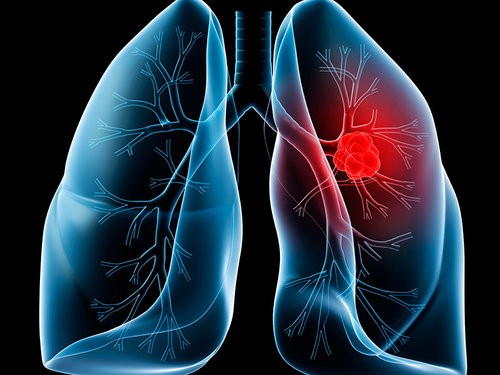
Early Detection of Lung Cancer
Lung cancer is the second most common cancer in both men and women, most people who develop lung cancer do not develop symptoms until it has become more advanced. In the case of late diagnosis, treatment can be effective, but rarely curative.
An effective screening test has long been desired for early detection with the goal of reducing mortality from lung cancer. Sputum cytology, chest radiography, and computed tomography (CT) scan have been studied as potential screening tests. The National Lung Screening Trial (NLST) demonstrated a 20% reduction in mortality with low-dose CT (LDCT) screening, and guidelines now endorse annual LDCT for those at high risk.
- Individuals who are 55-74 years of age.
- Individuals who have a minimum 30-pack-year history of smoking.
- Individuals who currently smoke.
- Individuals who have quit smoking in the past 15 years.
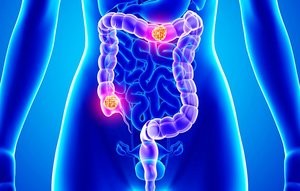
Early Detection of Colo-rectal Cancer
Colo-rectal Cancer is the third leading cause of cancer (excluding skin cancers). Risk factors include obesity, physical inactivity, excessive red meat and processed meat consumption, smoking and drinking alcohol.
There are several examinations to detect Colo-rectal cancer:
- Guaiac-based faecal occult blood test (gFOBT) and faecal immunochemical test (FIT): Samples of stool (faeces) are checked for blood, which might be a sign of a polyp or cancer.
- Stool DNA test: A sample of stool is checked for certain abnormal sections of DNA (genetic material) from cancer or polyp cells.
- Sigmoidoscopy: A flexible, lighted tube is put into the rectum and lower colon to check for polyps and cancer.
- Colonoscopy: A longer, flexible tube is used to look at the entire colon and rectum.
- Double-contrast barium enema: An x-ray test of the colon and rectum.
- CT colonography (virtual colonoscopy): This is a type of CT scan of the colon and rectum.
- Genetic testing: can help show whether the members of some families have inherited risk of developing Colo-rectal cancer because of inherited cancer symptoms such as Lynch syndrome (also known as non-polyposis Colo-rectal hereditary cancer, or HNPCC) or polyposis (FAP).
If you have a family history of polyps or colorectal cancer, you are more susceptible to colorectal cancer yourself. These risks can be higher in people who have a strong family history of colorectal cancer. While cancer in a document (first degree) relatives such as parents, brothers, and sisters are the most concerning, cancer in more distant relatives is also important. The presence of two or more of the relatives of people with colon and rectal cancer is more on the existence of only one, compared with her. It’s also more if your relatives have been diagnosed with cancer at a younger age than usual.
